Pain relief can significantly improve your quality of life, but it’s important to understand the various options available. One effective method is the use of injections for pain relief, which can target specific areas of discomfort, reduce inflammation, and offer long-lasting relief. Whether you’re dealing with chronic pain, acute injuries, or ongoing discomfort, injections could be a valuable part of your treatment plan. However, it’s essential to have a clear understanding of what these injections involve, how they work, and what you should consider before opting for this approach.
What Are Injections for Pain Relief?
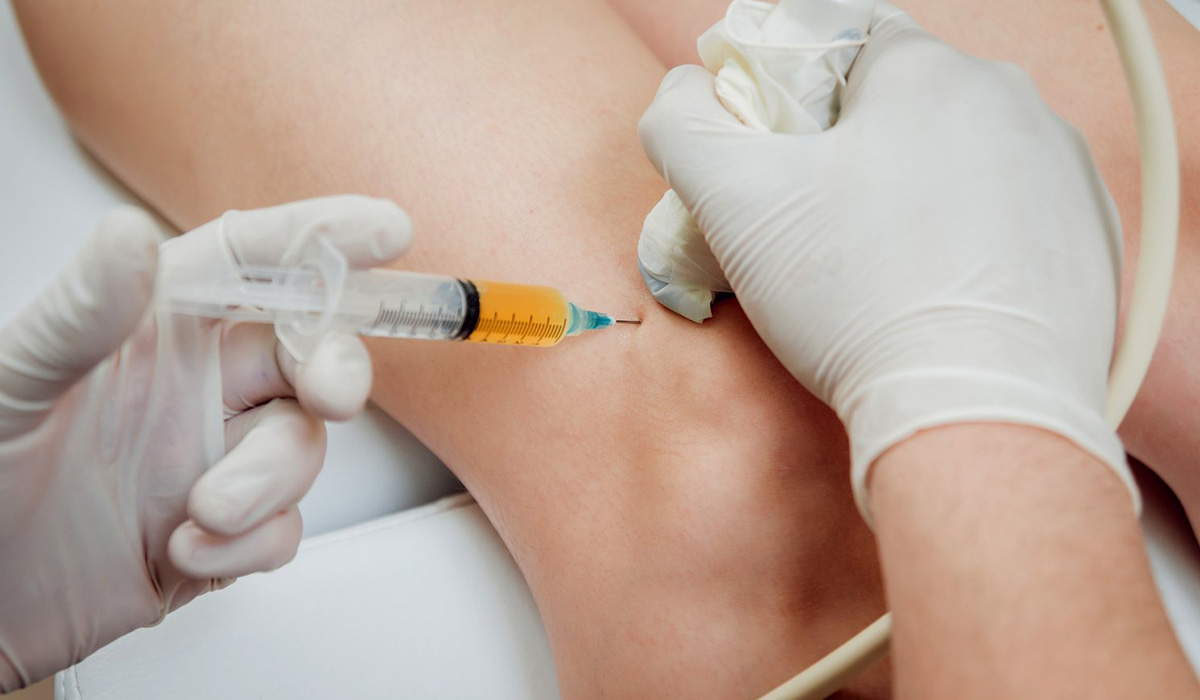
Injections for pain relief are medical procedures used to administer medication directly into or around the site of pain. These injections can deliver anti-inflammatory medications, corticosteroids, anesthetics, or other treatments designed to target specific conditions causing discomfort. The goal of these injections is to alleviate pain, reduce inflammation, and improve mobility without the need for invasive surgery.
There are several types of injections commonly used for pain relief:
- Corticosteroid Injections: These are often used to treat conditions that cause inflammation, such as arthritis, bursitis, and certain musculoskeletal disorders. Corticosteroids can help reduce swelling and relieve pain temporarily.
- Anesthetic Injections: These include local anesthetics that block nerve signals and can provide immediate pain relief. Nerve blocks, such as those used in chronic pain management, are common examples.
- Platelet-Rich Plasma (PRP) Injections: PRP therapy is gaining popularity for treating musculoskeletal injuries and conditions, such as tendonitis or arthritis. It involves using a sample of your own blood, which is processed to concentrate the healing components, and then injected into the affected area.
- Hyaluronic Acid Injections: These are used primarily for osteoarthritis and help improve lubrication in the joint, relieving stiffness and pain.
When Are Injections Recommended?
Injections for pain relief are often recommended when other treatment methods, such as medications, physical therapy, or lifestyle changes, haven’t been effective. Injections can be used for both acute and chronic pain conditions, and your healthcare provider may suggest injections in the following situations:
- Chronic Joint Pain: For conditions like osteoarthritis or rheumatoid arthritis, injections can reduce inflammation and slow down the progression of joint damage.
- Muscle and Tendon Injuries: Injections can help in cases of tendinitis, bursitis, or other soft tissue injuries by promoting healing and alleviating pain.
- Back Pain: Injections can be used to relieve lower back pain caused by conditions like herniated discs, spinal stenosis, or sciatica.
- Headaches: For migraines or tension headaches, specific injections can help manage symptoms.
What to Consider Before Receiving Injections?
Before opting for injections as a pain relief treatment, there are several important factors to consider:
- Medical History: Discuss your full medical history with your healthcare provider. It’s important to inform them about any underlying health conditions, previous injuries, or chronic diseases that could impact the success of the injections.
- Current Medications: Let your healthcare provider know about any medications you are currently taking, including over-the-counter drugs, supplements, and other prescription medications. This helps to avoid interactions that could interfere with the effectiveness of the injections.
- Allergies: If you have any known allergies—particularly to anesthetics, corticosteroids, or other medications—be sure to share this information with your provider.
- Potential Risks: Like all medical procedures, injections come with certain risks. These may include pain at the injection site, swelling, infection, or allergic reactions. Your healthcare provider will assess these risks based on your specific condition.
- Expected Outcomes: Understand what to expect from the injection. Injections can provide temporary relief, but they are not a cure. They are often part of a broader pain management plan that may include other therapies.
- Long-Term Management: Consider the long-term management of your condition. Injections may offer temporary relief, but long-term pain management may require a combination of treatments, lifestyle changes, and possibly more frequent injections.
What to Expect During the Procedure?
The process of receiving a pain relief injection typically involves the following steps:
- Consultation: You’ll first have a consultation with your healthcare provider to discuss your pain, medical history, and the best course of action.
- Preparation: Depending on the type of injection, you may be asked to stop certain medications or adjust your lifestyle in preparation for the procedure.
- The Injection: During the injection procedure, a trained healthcare provider will carefully target the area causing pain. This may involve the use of imaging techniques such as X-rays, ultrasound, or fluoroscopy to ensure accuracy. The procedure is usually done in a clinic setting and can be performed with local anesthesia.
- Recovery: After the injection, you may experience mild discomfort or swelling. Most people are able to resume their daily activities shortly after the procedure, but it’s important to follow your provider’s post-injection care instructions.
Long-Term Pain Management with Injections
While injections can offer relief in the short term, managing pain effectively often requires a combination of treatments. These may include physical therapy, lifestyle changes, medication adjustments, and other pain management strategies. In some cases, repeated injections may be necessary, but it’s important to work closely with your healthcare provider to develop a personalized treatment plan that balances relief with long-term care.
Nexus Advanced Pain Management: A Trusted Partner in Pain Relief
If you’re seeking expert guidance for pain relief, Nexus Advanced Pain Management offers comprehensive care that focuses on both immediate pain relief and long-term healing. With state-of-the-art facilities and a team of experienced pain specialists, Nexus Advanced Pain Management tailors treatment plans to each individual’s unique needs. Whether through injections, physical therapy, or other advanced pain management techniques, they are dedicated to helping patients regain their comfort and mobility.
At Nexus Advanced Pain Management, patients benefit from personalized care, cutting-edge technology, and a compassionate approach to pain relief. Their goal is not only to alleviate pain but also to empower patients with the knowledge and tools they need to live fuller, healthier lives.
Conclusion
Injections for pain relief can be an effective tool for managing both acute and chronic pain, offering targeted relief without the need for surgery. However, it’s crucial to have a thorough understanding of the options, consider the potential risks, and work closely with a healthcare provider to determine the most appropriate treatment plan for your specific needs. If you’re looking for expert pain management in your area, Nexus Advanced Pain Management stands out as a trusted partner, providing personalized and comprehensive care to help you find relief and restore your quality of life.